Grantee Research Project Results
2015 Progress Report: Long Term Metabolic Consequences of Exposures to Multipollutant Atmospheres in the Great Lakes Region
EPA Grant Number: R834797C003Subproject: this is subproject number 003 , established and managed by the Center Director under grant R834797
(EPA does not fund or establish subprojects; EPA awards and manages the overall grant for this center).
Center: Center for Research on Early Childhood Exposure and Development in Puerto Rico
Center Director: Alshawabkeh, Akram
Title: Long Term Metabolic Consequences of Exposures to Multipollutant Atmospheres in the Great Lakes Region
Investigators: Rajagopalan, Sanjay , Sun, Qinghua
Institution: The Ohio State University , University of Michigan
Current Institution: The Ohio State University
EPA Project Officer: Chung, Serena
Project Period: December 1, 2010 through November 30, 2015 (Extended to December 31, 2016)
Project Period Covered by this Report: August 1, 2014 through July 31,2015
RFA: Clean Air Research Centers (2009) RFA Text | Recipients Lists
Research Category: Human Health , Air
Objective:
We recently demonstrated that short-term exposure to inhaled concentrated airborne particulate (CAP) matter <2.5 µm (PM2.5) results in components of cardiometabolic syndrome (CMS) including development of hypertension and insulin resistance. In this project, we hypothesize that chronic inhalation of CAP in conjunction with gaseous components such as ozone from distinct multipollutant atmospheres synergistically interacts with diet and genetic susceptibility to influence development of CMS. Project 3 is an integral component of the overarching theme of this center that primary air pollutants, fine PM (PM2.5) and ozone (O3), cause cardiometabolic health effects that are dependent on the local atmospheric multipollutant milieu, predisposing factors, and the interactive toxicity of multipollutant coexposure. The experiments proposed are natural extensions of human research outlined in Project 1 and acute experiments in Project 2 and will focus on conducting chronic inhalation toxicology studies in diet fed and genetic models of obesity/diabetes. In Aim 1, simultaneous chronic exposure to multipollutant CAP from two locations in Columbus, OH, representing near-roadside/traffic or remotely transported/aged emissions will be examined in combination with high fat chow (HFC). The impact of CAP on glucose/insulin homeostasis, adipokines, insulin signaling, adipose and pulmonary inflammation and an analysis of dose dependence and CAP components most likely associated with these effects will be evaluated in diet sensitive (C57BL/6) and genetic models of Type II diabetes susceptibility (KKA/y). In Aim 2, we will investigate the effect of co-exposure of multipollutant CAP with ozone on the temporal development of insulin resistance and adipose/lung inflammation using the KKA/y model. We will assess dose response relationship of multipollutant-O3 mixture on insulin resistance measures (HOMA-IR and IPGTT) and novel mediators of innate immunity, pivotal in the development of metabolic derangement. Based on data from Aims 1 and 2, we will design experiments in Aim 3, which will help us assess chronic effects of multipollutant CAP in potentiating inflammatory monocyte activation and infiltration into tissue niches as a central mechanism for mediating adverse metabolic effects of CAP. Using state of the art multiple exposure systems available at OSU (OASIS-1 and OASIS-2) and MI in conjunction with the resources available at the ECC, including the use of several novel and novel high-time resolution exposure characterization methods, GLACIER offers an unprecedented opportunity to elucidate relevant mechanisms responsible for the effects of multipollutant CAP on the pathogenesis of insulin resistance and inflammation. The insights gleaned from the acute studies planned in Projects 1 and 2 in conjunction with chronic studies in Project 3, have significant public health ramifications and may eventually lead to policy changes to avert environmental exposure to PM2.5.
Progress Summary:
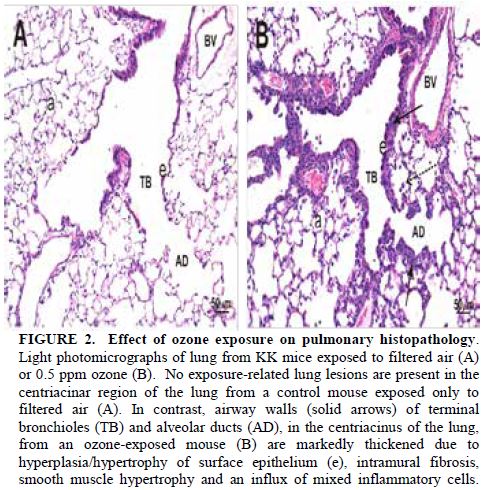
In our prior years of funding for this aim, we successfully conducted experiments to determine the temporal course of diabetes development in response to ozone and reported these results in several manuscripts in collaboration with Dr. Harkema. We were interested in isolating the effects of ozone prior to conducting multipollutant exposures in combination with CAPS, which we had proposed performing as part of Aim 3 as data from our groups appeared to suggest seemingly opposing effects. Inhalation exposure to O3 was conducted in whole-body exposure chambers, and KK mice were exposed to nominal ozone concentrations of 0 (filtered room air), or 0.5 ppm, for 8 h/d, 7 d/wk for 13 wk (n = 8/group). Ozone was generated with two OREC Model OZONEV1-O ozonizers (Ozone Research and Equipment Corp., Phoenix, AZ), with compressed air used as a source of oxygen. The concentration of ozone within the chambers was monitored throughout the exposure with three Dasibi 1003 AH ambient-air ozone monitors (Dasibi Environmental Corp., Glendale, CA). The air-sampling probes were placed in the breathing zone of the mice. The chamber ozone concentration was automatically maintained through a computer-controlled closed-loop feedback system, which adjusted the amount of ozone delivered to the chamber through remotely controlled mass-flow valves. After three weeks of inhalation exposure to control air or ozone, mice were sacrificed. The weights of whole body and organs were recorded and metabolic as well as inflammation were examined. Figures 1 and 2 depict the effect of ozone exposure on lung inflammation. The total inflammatory cells in the bronchoalveolar lavage fluid (BALF) increased by ~3-fold (Figure 1A) and cellular component analysis suggested macrophage, neutrophil, eosinophil, and lymphocytes all increased (Figure 1B).
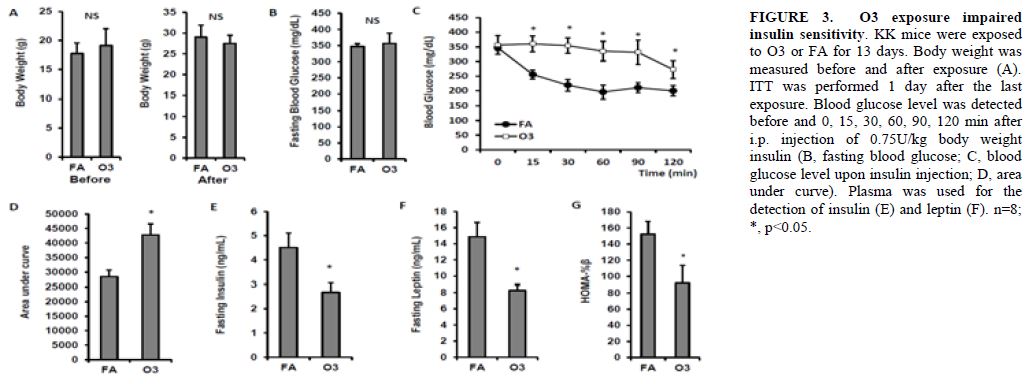
Histological examination confirmed the infiltration of immune cells in the airway. Ozone-exposed KK mice had pulmonary histopathology that was restricted to centriacinar regions throughout the lung lobe compared to FA-exposed mice (Figures 2A & 2B). These ozone-induced lung lesions were morphologically characterized by marked thickening of terminal bronchioles and proximal alveolar ducts as a result of hyperplasia/hypertrophy of surface epithelium, intramural fibrosis, smooth muscle hypertrophy and a mixed inflammatory cell infiltrate (i.e., mononuclear cells, neutrophils and eosinophils; bronchiolitis/alveolitis). Conspicuous aggregates of monocytes/macrophages and lesser numbers of other inflammatory cells (i.e., neutrophils, eosinophils, and lymphocytes) also were present in centrinacinar airspaces. No exposure-related histopathology was found in the lungs of KK mice exposed only to filtered air (Figure 2A). These results are depicted in Figure 2. After 3 weeks of exposure, there were no differences in body weight between the O3- and FA-exposed animals (Figure 3A). Although no significant difference in fasting blood glucose was observed between FA- and O3-exposed animals (Figure 3B), three-week O3 exposure significantly impaired insulin sensitivity in KK mice (Figure 3C & 3D, p<0.05). Fasting plasma insulin levels were lower in O3-exposed mice (4.5 ± 0.6 ng/mL vs. 2.7 ± 0.4 ng/mL for FA vs. O3, p<.05, Figure 3E). Consistent with these observations, fasting plasma leptin level and HOMA-beta were also reduced after O3 exposure in KK mice (Figures 3F & 3G).
To investigate the impact of O3 inhalation on immune response, macrophage and CD4+ T cell population were quantified using flow cytometry. Monocytes were characterized by the expression CD11b and F4/80 in mice (Geissmann, et al., 2003). As depicted in Figures 4A, CD11b+ F4/80+ monocytes increased in blood (6.5 ± 0.1% vs. 7.9 ± 0.6% for FA vs. O3) although no statistical significance was observed (p=0.06). CD4+ T cell percentage in blood was lower in O3-exposed mice (14.3 ± 0.6% vs. 10.8 ± 0.6% for FA vs. O3, p=0.001, Figure 4B). Infiltration of adipose tissue macrophage (ATM) increased in epididymal fat of KK mice exposed to O3 (37.9 ± 1.2% vs. 44.3 ± 2.1% for FA vs. O3, p=0.02, Figure 4C) and percentage of CD4+ T cell decreased in epididyma fat of O3-exposed KK mice (1.2 ± 0.08% vs. 0.9 ± 0.08% for FA vs. O3, p=0.04, Figure 4D).
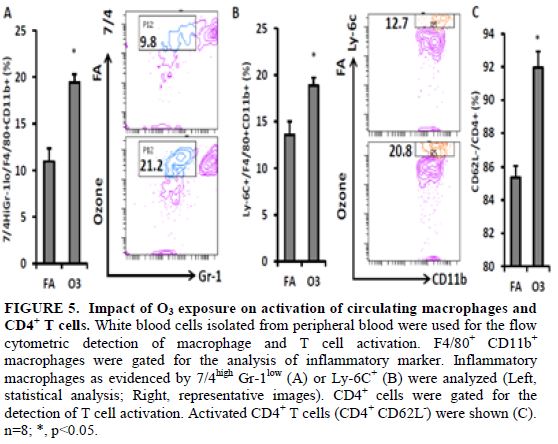
Next, we detected the activation of monocytes and CD4+ T cells in the blood of O3-exposed KK mice. Gr1low 7/4high inflammatory monocytes were significantly increased in the circulation of KK mice exposed to O3 (11.0 ± 1.3% vs. 19.4 ± 0.9% for FA vs. O3, p<0.001, FIGURE 5A). To confirm this result, we used another marker Ly-6C to identify inflammatory monocytes. Ly6C+ monocyte level in circulation was higher in O3-exposed mice compared with that in FA-exposed mice (13.6 ± 1.4% vs. 18.9 ± 0.8% for FA vs. O3, p=0.006, Figure 5B). The activated CD4+ T cells (CD4+ CD62L-) also increased after O3 exposure (85.4 ± 0.7% vs. 92.0 ± 1.0% for FA vs. O3, p<0.001, Figure 5C).
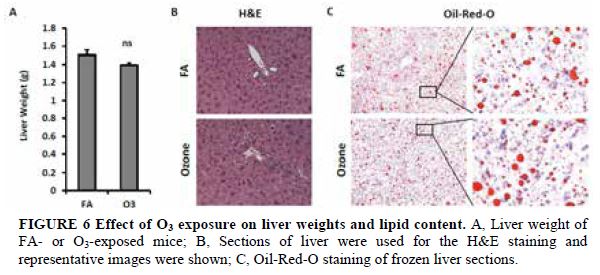
As depicted in Figure 6A, KK mice exposed to O3 and FA had similar liver weights. H&E staining shows normal liver architecture and morphology in mice exposed to O3 (Figure 6B). To investigate whether O3 exposure affects hepatic lipid content, liver frozen sections were used for Oil-Red-O staining. As shown in Figure 6C, similar levels of lipid content were observed in liver of mice exposed to FA and O3.
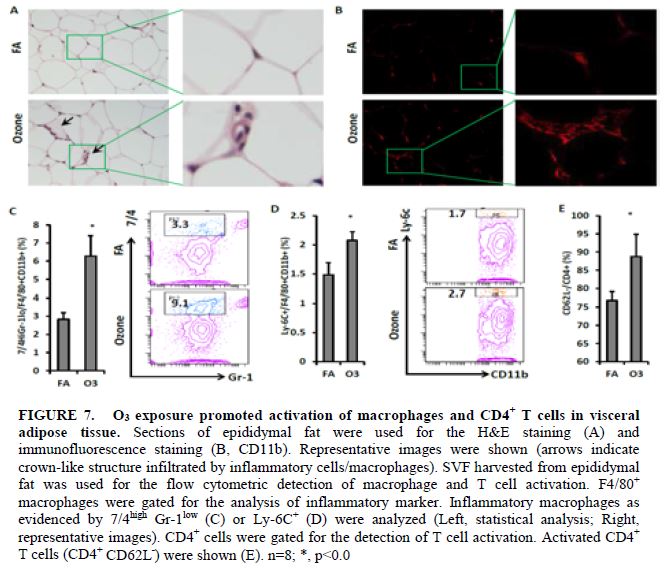
To investigate inflammatory cell infiltration in visceral adipose tissue, epididymal fat tissues from exposed mice were used for the H&E staining and Mac-1 immunofluorescence staining. More crown-like structures (infiltration of inflammatory cells) were observed in the epididymal fat of O3-exposed mice (Figures 7A & 7B). Consistent with the observations in blood, infiltration of inflammatory macrophages in visceral adipose tissue was enhanced by O3 exposure. As shown in Figure 7C, percentage of Gr-1low 7/4high macrophage increased in the epididymal fat of O3-exposed mice (2.8 ± 0.4% vs. 6.3 ± 1.1% for FA vs. O3, p=0.02,). Ly-6C+ macrophage infiltration in the epididymal fat of O3-exposed mice is also higher than that of mice exposed to FA (1.5 ± 0.2% vs. 2.1 ± 0.2% for FA vs. O3, p=0.04, Figure 7D). There was also an increased activation of CD4+ T cell in the adipose tissue of O3-exposed KK mice (76.8 ± 2.3% vs. 88.8 ± 6.1% for FA vs. O3, p<0.001, Figure 7E).
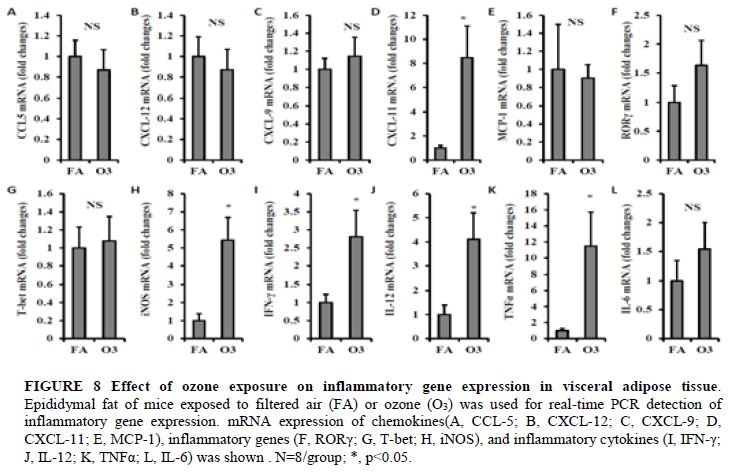
To investigate the impact of ozone inhalation on immune activation in adipose tissue, we next detected the mRNA expression level of chemokines, proinflammatory cytokines, and inflammatory genes in visceral adipose tissue. No significant difference in CCL-5, CXCL-12, CXCL-9, MCP-1, RORγ, Tbet and IL-6 were observed between FA and O3-exposed mice (Figures 8A-C, 8E-G, and 8L). Expression of CXCL-11 was increased by 8.5-fold in animals exposed to O3 (1.0 ± 0.22 vs. 8.5 ± 2.63 for FA vs. O3, p=0.02, Figure 8D). There were also a 5.4-fold increase of iNOS (1.0 ± 0.39 vs. 5.4 ± 1.26 for FA vs. O3, p=0.007, Figure 8H), 2.8-fold increase of IFN-γ (1.0 ± 0.23 vs. 2.8 ± 0.73 for FA vs. O3, p=0.045, Figure 8I), 4.1-fold increase of IL-12 (1.0 ± 0.40 vs. 4.1 ± 1.10 for FA vs. O3, p=0.026, Figure 8J), and 11.5-fold increase of TNFα (1.0 ± 0.24 vs. 11.5 ± 4.24 for FA vs. O3, p=0.039, Figure 8K).
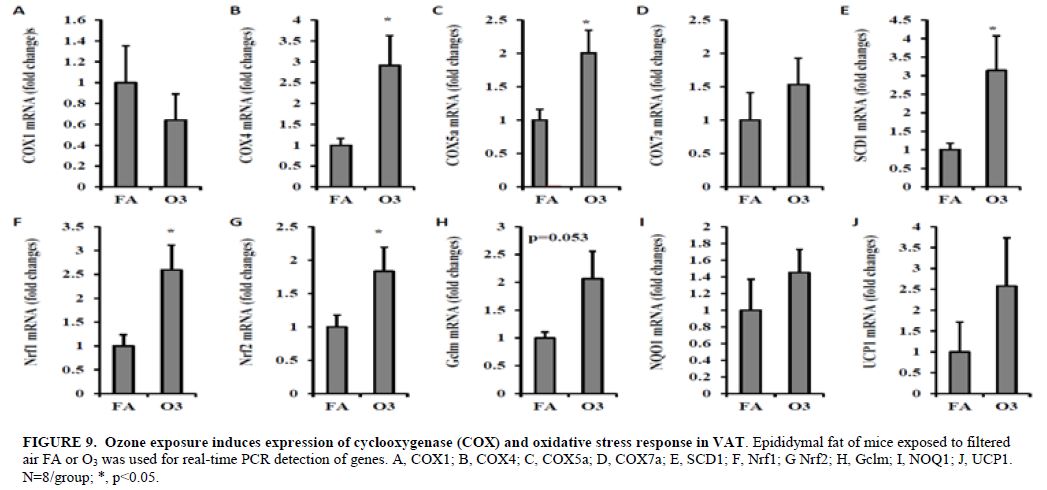
To investigate whether oxidative stress plays a role in ozone exposure, we detected the expression of genes involved in oxidative stress. As depicted in Figure 9, multiple oxidative stress-related genes including COX4 (1.0 ± 0.16 vs. 2.9 ± 0.71 for FA vs. O3, p=0.021, Figure 9B), COX5α (1.0 ± 0.16 vs. 2.0 ± 0.34 for FA vs. O3, p=0.016, Figure 9C), SCD1 (1.0 ± 0.18 vs. 3.1 ± 0.93 for FA vs. O3, p=0.041, Figure 9E), Nrf1 (1.0 ± 0.24 vs. 2.6 ± 0.52 for FA vs. O3, p=0.014, Figure 9F), and Nrf2 (1.0 ± 0.17 vs. 1.8 ± 0.36 for FA vs. O3, p=0.045, Figure 9G) were up-regulated by the exposure of O3. These results seem to suggest a dissociation of measures of inflammation in the circulation and tissue niches such as adipose from systemic insulin resistance in the context of a lean phenotype. This is to our knowledge the first description of a phenotype where there were seemingly reciprocal effects on inflammation and insulin resistance. Our results further seemed to suggest that the effects of ozone in conjunction with PM2.5 may indeed be complex with prediction of a phenotype rendered difficult by these opposing influences. These data indicate that the combined effects of a mixture may be far more complex than a simple additive or synergistic interaction. We have further examined Akt phosphorylation levels in liver and skeletal muscle and found that ozone-exposed animals had significantly increased Akt phosphorylation levels in liver and skeletal muscle but not in adipose tissues, suggesting that ozone exposure increases insulin sensitivity in hyperglycaemic KKAy mice. In our experiments for the coming year we plan on performing experiments with co-exposure with careful assessment of the phenotypes of individual component exposure to compare and contrast the effect of co-exposure.
Future Activities:
All aspects of the study protocol are approved by our IACUC. We anticipate beginning our CAPS + Ozone exposure this year.Journal Articles on this Report : 15 Displayed | Download in RIS Format
| Other subproject views: | All 45 publications | 34 publications in selected types | All 34 journal articles |
|---|---|---|---|
| Other center views: | All 148 publications | 72 publications in selected types | All 72 journal articles |
| Type | Citation | ||
|---|---|---|---|
|
|
Blazek A, Rutsky J, Osei K, Maiseyeu A, Rajagopalan S. Exercise-mediated changes in high-density lipoprotein: impact on form and function. American Heart Journal 2013;166(3):392-400. |
R834797 (2013) R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2013) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit |
|
|
Liu C, Ying Z, Harkema J, Sun Q, Rajagopalan S. Epidemiological and experimental links between air pollution and type 2 diabetes. Toxicologic Pathology 2013;41(2):361-373. |
R834797 (2013) R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C002 (2012) R834797C002 (2013) R834797C002 (2014) R834797C002 (2015) R834797C002 (2016) R834797C002 (Final) R834797C003 (2013) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Liu C, Xu X, Bai Y, Wang TY, Rao X, Wang A, Sun L, Ying Z, Gushchina L, Maiseyeu A, Morishita M, Sun Q, Harkema JR, Rajagopalan S. Air pollution-mediated susceptibility to inflammation and insulin resistance:influence of CCR2 pathways in mice. Environmental Health Perspectives 2014;122(1):17-26. |
R834797 (2013) R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C002 (2014) R834797C002 (2015) R834797C002 (2016) R834797C002 (Final) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
|
|
|
Liu C, Bai Y, Xu X, Sun L, Wang A, Wang TY, Maurya SK, Periasamy M, Morishita M, Harkema J, Ying Z, Sun Q, Rajagopalan S. Exaggerated effects of particulate matter air pollution in genetic type II diabetes mellitus. Particle and Fibre Toxicology 2014;11:27. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C002 (2014) R834797C002 (2015) R834797C002 (2016) R834797C002 (Final) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Liu C, Fonken LK, Wang A, Maiseyeu A, Bai Y, Wang T-Y, Maurya S, Ko Y-A, Periasamy M, Dvonch T, Morishita M, Brook RD, Harkema J, Ying Z, Mukherjee B, Sun Q, Nelson RJ, Rajagopalan S. Central IKKβ inhibition prevents air pollution mediated peripheral inflammation and exaggeration of type II diabetes. Particle and Fibre Toxicology 2014;11:53. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Morishita M, Bard RL, Kaciroti N, Fitzner CA, Dvonch T, Harkema JR, Rajagopalan S, Brook RD. Exploration of the composition and sources of urban fine particulate matter associated with same-day cardiovascular health effects in Dearborn, Michigan. Journal of Exposure Science & Environmental Epidemiology 2015;25(2):145-152. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C001 (2014) R834797C001 (2015) R834797C001 (2016) R834797C001 (Final) R834797C002 (2014) R834797C002 (2015) R834797C002 (2016) R834797C002 (Final) R834797C003 (2015) R834797C003 (Final) |
Exit Exit |
|
|
Morishita M, Bard RL, Wang L, Das R, Dvonch JT, Spino C, Mukherjee B, Sun Q, Harkema JR, Rajagopalan S, Brook RD. The characteristics of coarse particulate matter air pollution associated with alterations in blood pressure and heart rate during controlled exposures. Journal of Exposure Science & Environmental Epidemiology 2015;25(2):153-159. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C001 (2014) R834797C001 (2015) R834797C001 (2016) R834797C001 (Final) R834797C002 (2015) R834797C002 (2016) R834797C002 (Final) R834797C003 (2015) R834797C003 (Final) R833740 (Final) |
Exit Exit |
|
|
Newby DE, Mannucci PM, Tell GS, Baccarelli AA, Brook RD, Donaldson K, Forastiere F, Franchini M, Franco OH, Graham I, Hoek G, Hoffmann B, Hoylaerts MF, Kunzli N, Mills N, Pekkanen J, Peters A, Piepoli MF, Rajagopalan S, Storey RF, ESC Working Group on Thrombosis, European Association for Cardiovascular Prevention and Rehabilitation, ESC Heart Failure Association. Expert position paper on air pollution and cardiovascular disease. European Heart Journal 2015;36(2):83-93b. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Rajagopalan S, Brook RD. Personalizing your airspace and your health. Journal of the American College of Cardiology 2015;65(21):2288-2290. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Rao X, Zhong J, Maiseyeu A, Gopalakrishnan B, Villamena FA, Chen LC, Harkema JR, Sun Q, Rajagopalan S. CD36-dependent 7-ketocholesterol accumulation in macrophages mediates progression of atherosclerosis in response to chronic air pollution exposure. Circulation Research 2014;115(9):770-780. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C002 (2015) R834797C002 (Final) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Rao X, Patel P, Puett R, Rajagopalan S. Air pollution as a risk factor for type 2 diabetes. Toxicological Sciences 2015;143(2):231-241. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Rao X, Montresor-Lopez J, Puett R, Rajagopalan S, Brook RD. Ambient air pollution:an emerging risk factor for diabetes mellitus. Current Diabetes Reports 2015;15(6):603. |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2015) R834797C003 (Final) |
Exit Exit |
|
|
Ying Z, Xu X, Chen M, Liu D, Zhong M, Chen L-C, Sun Q, Rajagopalan S. A synergistic vascular effect of airborne particulate matter and nickel in a mouse model. Toxicological Sciences 2013;135(1):72-80. |
R834797 (2013) R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
Exit Exit Exit |
|
|
Ying Z, Xu X, Bai Y, Zhong J, Chen M, Liang Y, Zhao J, Liu D, Morishita M, Sun Q, Spino C, Brook RD, Harkema JR, Rajagopalan S. Long-term exposure to concentrated ambient PM2.5 increases mouse blood pressure through abnormal activation of sympathetic nervous system:a role for hypothalamic inflammation. Environmental Health Perspectives 2014;122(1):79-86. |
R834797 (2013) R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C002 (2013) R834797C002 (2014) R834797C002 (2015) R834797C002 (2016) R834797C002 (Final) R834797C003 (2013) R834797C003 (2014) R834797C003 (2015) R834797C003 (Final) |
|
|
|
Ying Z, Xie X, Bai Y, Chen M, Wang X, Zhang X, Morishita M, Sun Q, Rajagopalan S. Exposure to concentrated ambient particulate matter induces reversible increase of heart weight in spontaneously hypertensive rats. Particle and Fibre Toxicology 2015;12:15 (10 pp.). |
R834797 (2014) R834797 (2015) R834797 (2016) R834797 (Final) R834797C003 (2015) R834797C003 (Final) |
Exit Exit |
Supplemental Keywords:
ozone, O3, PM2.5, type II diabetes mellitus, DM, insulin resistance;, Air, Scientific Discipline, ENVIRONMENTAL MANAGEMENT, Health Risk Assessment, Biology, Biochemistry, air toxics, Risk Assessment, aerosol particles, physiology, human exposure, particulate matter, cardiotoxicity, susceptible populations, acute cardiovascualr effects, ambient air quality, cardiopulmonaryRelevant Websites:
GLACIER: Great Lakes Air Center For Integrated Environmental Research Exit
Progress and Final Reports:
Original AbstractMain Center Abstract and Reports:
R834797 Center for Research on Early Childhood Exposure and Development in Puerto Rico Subprojects under this Center: (EPA does not fund or establish subprojects; EPA awards and manages the overall grant for this center).
R834797C001 Cardiometabolic Effects of Exposure to Differing Mixtures and Concentrations of PM2.5 in Obese and Lean Adults
R834797C002 Cardiometabolic, Autonomic, and Airway Toxicity of Acute Exposures to PM2.5 from Multipollutant Atmospheres in the Great Lakes Region
R834797C003 Long Term Metabolic Consequences of Exposures to Multipollutant Atmospheres in the Great Lakes Region
The perspectives, information and conclusions conveyed in research project abstracts, progress reports, final reports, journal abstracts and journal publications convey the viewpoints of the principal investigator and may not represent the views and policies of ORD and EPA. Conclusions drawn by the principal investigators have not been reviewed by the Agency.
Project Research Results
- Final Report
- 2016 Progress Report
- 2014 Progress Report
- 2013 Progress Report
- 2012 Progress Report
- 2011 Progress Report
- Original Abstract
34 journal articles for this subproject
Main Center: R834797
148 publications for this center
72 journal articles for this center