Grantee Research Project Results
Final Report: Novel Immunological Approaches to Link Ambient Air Pollution Exposure to Health Outcomes
EPA Grant Number: R834786Title: Novel Immunological Approaches to Link Ambient Air Pollution Exposure to Health Outcomes
Investigators: Nadeau, Kari
Institution: Stanford University
EPA Project Officer: Hahn, Intaek
Project Period: January 1, 2011 through December 31, 2013
Project Amount: $250,000
RFA: Exploring Linkages Between Health Outcomes and Environmental Hazards, Exposures, and Interventions for Public Health Tracking and Risk Management (2009) RFA Text | Recipients Lists
Research Category: Air Quality and Air Toxics , Human Health
Objective:
The overall goal of this research is to further understand the link between indicators of exposure and outcomes on human health by studying immune system changes in subjects exposed to elevated levels of ambient air pollution. We hypothesize that immunological indicators linked to environmental exposure and health outcomes will elucidate the role and mechanism of air pollution in asthma, a link which is theoretically understood, circumstantially clear, but not yet proven. We have developed a comprehensive novel indicator of hazard exposure that can be performed on one drop of blood. We will correlate cellular, serological, and epigenetic biomarker changes in peripheral blood, which can be broadly applied to an individual health outcome. The objectives of the research are (1) to examine the link between specific immune indicators and ambient air pollution exposure (level of exposure, chronicity of exposure, and type of exposure: ozone, NO/NO2, CO, PM2.5, PM10, sulfate, elemental carbon, polyaromatic hydrocarbons, daily naphthalene, endotoxin, fungal spores, and/or pollens) through a database collected in a large population in Fresno, CA. and (2) to characterize the relationship between immune indicators and health outcomes of asthma. Our approach was to examine asthma outcomes via a comprehensive collection of environmental exposure data through an established 8-year cohort study, the Fresno Asthmatic Children's Environmental Study (FACES) (n = 116 total). Health outcome data, individual estimate exposure levels, and blood sample results collected longitudinally from each subject were compared. The proposed research addresses the need to research the linkage between immune indicators, environmental exposure, and health outcomes. We expect that the resulting indicators from our blood sample analyses was characterized to allow for tracking of the impact of environmental health decisions and policy changes over time and in different locations. Our study also could lead to important mechanistic explanations of environmental exposures on human health. The results of the proposed research could provide indicators for long-term tracking and surveillance of environmental public health.
Summary/Accomplishments (Outputs/Outcomes):
The work on the project aims has proceeded smoothly and at the pace anticipated. All has progressed according to timelines, and all subjects have been recruited and are enrolled in the study. We have performed all cellular and molecular analyses on the blood samples obtained from the subjects. Results have been documented and publications have occurred and these are detailed below. The aims of the project did not change. They are:
Specific Aim 1: To explore whether the Treg immunological indicators are correlated with ambient air pollution exposure
Rationale and Hypothesis: The Fresno Asthma Children’s Environmental Study (FACES) is a cohort in which multiple environmental exposures and health outcomes are measured to determine whether exposure to ambient air pollution and bioaerosols are associated over the long-term with asthma in children and the extent to which these adverse outcomes are enhanced in asthmatic children who are allergic. My preliminary data suggest that children with allergic asthma have the most compromised Treg function. In addition, preliminary data suggest that Treg isolated from children have decreased expression of chemokines like CCL1, which are critically important for Treg chemotaxis to the lung. Thus, my first corollary hypothesis is that longitudinally collected Treg from children with asthma who are exposed to ambient air pollution will have profound dysfunction due to decreases in protein expression of FoxP3 and CCL1. My laboratory has developed a novel and innovative technique to create an immunological indicator to link immune cell changes to environmental exposure and health outcomes.
A. Examine whether levels and types of personal exposure to ambient air pollution measured 12 months prior to entry in the cohort are associated with worsened Treg impairment (through flow cytometry of Treg proteins, identification of CCL1 expression, fluid assays on plasma, and epigenetic studies of FoxP3).
B. Assess whether levels and types of personal exposure to ambient air pollution measured 12 months prior to entry in the cohort are associated with severity of asthma.
Specific Aim 2: To evaluate whether the Treg immunological indicators correlate with asthma health outcomes
Rationale and Hypothesis: Data show that Treg isolated from children with high exposure to ambient air pollution have decreased IL-10 and TGF-b; both are secreted in the plasma by Treg and are associated with immune tolerance in children. Decreased Treg numbers and Treg function have been associated with the onset of asthma and of allergy; moreover, decreased Treg occur with exacerbations of asthma. My second corollary hypothesis is that Treg exposed to high levels of ambient air pollution was impaired in their ability to regulate inflammation, which is manifest in children as more severe asthma health outcomes. Using samples from the FACES cohort, I will:
A. Determine whether Treg immunological indicators (through flow cytometry of Treg proteins, identification of CCL1 expression, fluid assays, and epigenetic studies of FoxP3) of attenuation of function correlate with severity of asthma through studies on asthmatic children.
B. Determine whether Treg immunological indicators of attenuation of function may help in the prediction of the likelihood of onset of asthma through studies on non-asthmatic children.
Overall Impact: The proposal is aimed to innovatively examine whether chronic ambient air exposures, the health outcomes of individual children, and changes in the immune system are correlated. The results are essential for understanding immune mechanisms that could be related to exposure and health outcomes. Overall, the results would help in decreasing and preventing the burden of asthma and allergy and reducing exposure to air pollution.
Results documented in the project (output). Our data demonstrate:
- that DNA methylation of the Foxp3 gene results in decreased FoxP3 protein levels in Treg and that the levels of FoxP3 decrease are associated with increases in levels of exposure to polycyclic aromatic hydrocarbons;
- that downregulation of chemokine receptor/cognate ligand pairs (CCR8/CCL1) is worsened by exposure to polycyclic aromatic hydrocarbons;
- that decreases in Treg-associated (TGF-b and IL-10) and increases in Th2-associated plasma markers (IL-4 and IL-13) correlate with increased levels of exposure to ambient air pollution;
- that higher degrees of Treg impairment correlate with severity of asthma; and
- that lower levels of Treg immune indicators can be detected in non-asthmatic children exposed to elevated levels of ambient air pollution.
The potential benefits of the results (outcomes). We expect our results to:
- provide sufficient evidence to help understand the link between the environmental hazard, exposure (individual estimate exposures), and the health outcomes (asthma) through the database collected in a large population in Fresno,CA;
- characterize the relationship between ambient air pollution exposure and biomarkers that can be used to indicate the health outcomes of asthma;
- be applicable and generalizable to other environmental circumstances (hazard exposure in different media at a diverse range of geographical locations in all ages sampled) since Treg as immunological indicators are associated with other diseases (cancer, autoimmunity, prematurity), since they are present at all stages of human development, and since they can be easily detected in blood samples; and
- be used in the future for long-term monitoring since the long-term effects of exposure to increased levels of ambient pollutants has become a major focus for population risk assessment and management in the setting of air quality standards. The immune indicator focus of this study could contribute in a major way to the lack of data in this area since it is not only important in longitudinal studies but also cross-generational studies (i.e., epigenetic studies of Foxp3 gene methylation patterns).
Conclusions:
Results:
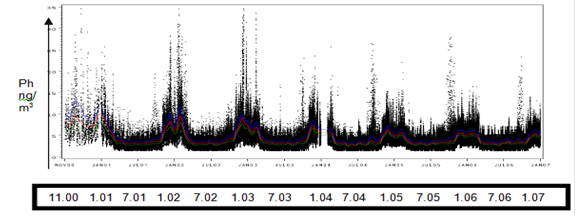
i) Air pollution modeling in Fresno. Our group has determined detailed individual exposure estimates over the past 9 years, using a microenvironment model which estimates daily personal exposure to pollutants of outdoor origin for each individual child in the study, accounting for variation between children in their home and school addresses. Data generated using our individual estimate exposure model are shown in Figure 1. PAH (primarily phenanthrene and naphthalene) peak in mid-January.
Figure 1: Daily personal exposure measurements of a PAH (ambient phenanthrene) in (ng/m3), November 2000 (11.00) - January 2007 (1.07), for N = 312 FA children. Green, red, and blue solid lines indicate 25th percentile, median, and 75th percentile values, respectively.
ii) Air pollution and Foxp3 methylation. Recently, we showed that in asthmatic subjects (n = 71) who resided in Fresno, CA, there was a direct relation between higher levels of ambient polycyclic aromatic hydrocarbon (PAH) exposure and greater methylation in the Foxp3locus, that, in turn, was associated with the most severe impairment of Treg function and the most severe phenotypes of clinical asthma outcomes (as measure by GINA score). We measured other exposures and AAP toxicants (i.e., endotoxin, pollens, molds, ozone, NO2, carbon monoxide, PM2.5, PM10, and elemental carbon) but did not show any significant associations with Foxp3 transcript expression in Treg, or Treg function (p > 0.12, r2 < 0.04 for each association tested).
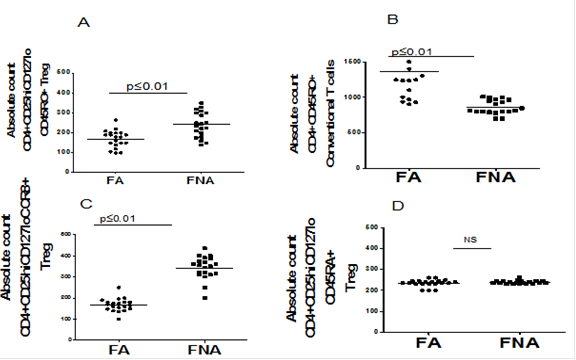
iii) CD45RO+Treg are decreased in FA subjects. Based on experiments in which we calculated the absolute numbers of live Treg and effector CD4+ T cell for each subject sample, we found that the CD45RO+ (adaptive or short-lived) Treg from FA subjects were lower in absolute numbers (Figure 2A) compared to FNA. CD45RO+ (memory) conventional T cells were increased in the FA population (Figure 2B), indicating the possible conversion of CD45RO+Treg into CD45RO+ conventional CD4+ T cells in vivo. Our laboratory has confirmed that these are memory Treg via other memory cell markers (i.e., CD62Llo, CD44hi, HLA-DRhi; data not shown).
These results show the feasibility of identifying different subsets within the Treg population by the high resolution immunophenotyping methods performed in my laboratory. The results suggest that low numbers of CD45RO+CD45RA- Treg in FA subjects might play a role in asthma in those exposed to AAP. It is important to note that the CD45RA+CD45RO- Treg population remained similar in all groups (Figure 2D). The CD45RA+ subset has been shown to maintain self-tolerance and prevent autoimmune diseases56, 66-68; therefore, with these findings, it is possible that a susceptibility to autoimmune disease would not occur in the FA subjects.
Figure 2. Low numbers of memory Treg in Fresno Asthmatic (FA) Cohort. Multicolor flow cytometry performed (LSR II, BD Biosciences) on less than 500 mL whole blood stained with antibodies and cells were gated for: (A) CD45RO+ Treg in FA (n = 20), FNA (n = 20); (B) CD4+CD45RO+ T cells in FA (n = 20), FNA (n = 20); (C) CCR8+ Treg in FA (n = 20), FNA (n = 20), (D) CD45RA+Treg in Treg in FA (n = 20), FNA (n = 20). CBC with differential was used with % of each subset to determine absolute numbers (cells/mL). P values ≤ 0.05 represented significant differences from one-way ANOVA using non-parametric Kruskall-Wallis Test and pairwise post-test comparisons via Dunns multiple comparison test.
iv) Treg migration to the primary bronchial epithelial cells is impaired in FA. My laboratory and others have shown that Treg are decreased in number and in function in BAL of patients with allergic asthma compared to controls. We and others have determined that Treg express specific chemokine receptors (CCR4 and CCR8) to respond to ligands produced by human bronchial epithelial cells (HBEC) (i.e., CCL17, CCL22). Since we found low Foxp3 levels in the FA cohort studied to date, we hypothesized that Treg would have less CCR4 or CCR8 and therefore, migration of Treg to primary HBEC (Promocell, Germany) would be impaired. Our preliminary data show reduced migration of Treg from FA subjects and we found that Treg from FA subjects had decreased CCR8 protein expression compared to FNA subjects. This decrease could hinder the effective migration to lung epithelium of Treg and thereby limit their suppression of CD4+ T-cell proliferation, thus possibly worsening asthma outcomes (Figure 2C).
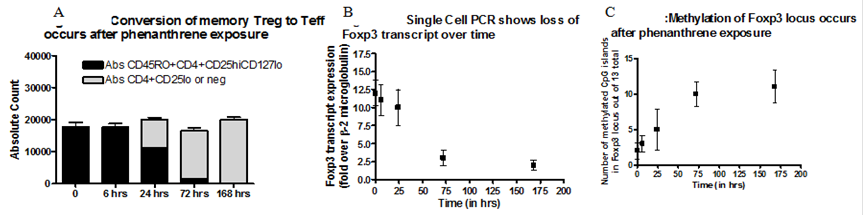
v) In vitro preliminary studies dissecting upstream and downstream pathways involved in PAH exposure: To begin to further explore the biological mechanisms of PAH exposure on Treg, we chose to study the in vitro effects of phenanthrene, one of the most elevated ambient PAH species measured in Fresno, CA, on the Foxp3 genetic locus. Other combinations of PAH species and Treg-associated genes was evaluated in the future. Data in children exposed to chronic, high levels of phenanthrene demonstrate a mean serum concentration of 2.0 mM, we chose a 10-fold higher concentration for our in vitro work performed over 7 days, similar to other publications using PAH in in vitro cellular assays.
Figure 3: In vitro conversion of memory Treg to Teff cells occurs with methylation of the Foxp3 gene locus. Flow cytometry-purified memory Treg (to over 99% purity) from a representative healthy control were incubated with phenanthrene (20.0 mM) dissolved in 10-2 M DMSO (dimethylsulfoxide) in complete RPMI media. Vertical bars represent standard deviation from the mean of n = 8 repeats for each condition. Conversion to a memory conventional CD4+ T cell occurred in vitro (A). As a control, DMSO at 10-2 M in media did not have any effect on conversion of Treg into Teff cells (data not shown). Single-cell PCR was performed (Fluidigm, CA) and loss of Foxp3 transcripts over time after phenanthrene exposure (20.0 mM) is shown below (B). When flow cytometry-purified Treg from healthy controls were used in standard autologous suppression assays using methods published by my laboratory, after incubation with phenanthrene (20.0 mM) vs. DMSO control, there was 60% Treg function impairment vs, 91% Treg function (p<0.01)(not shown). Sequencing of 13 CpG islands of the Foxp3 promoter and intron regions occurred using methods we have published and increased methylation over time was present after phenanthrene (20.0 mM) (C) but not for the DMSO control. Naïve (CD45RA+ Treg) were less susceptible to the effects of phenanthrene in all in vitro assays performed (not shown).
Although unlikely, it is possible that a 1% or less contaminant of Teff in our flow cytometry-purified Treg were expanded after phenanthrene exposure, and therefore, the increase over time in Teff was due to increased proliferation rather than Treg conversion to Teff. To test this, we incubated Teff alone (2,000 absolute count, representing approximately 1% from our assay in Figure 3A) with phenanthrene at 20.0 mM over 7 days. No significant increase in proliferation of Teff cells was detected (data not shown).
We further interrogated the dependence of our cellular and molecular finding on the AhR since PAH is known to be a ligand for AhR76. Specifically, we used gene silencing techniques (Neon, Invitrogen, CA) with siRNA to AhR in flow cytometry-purified Treg from healthy controls using published methods and demonstrated the abrogation of methylation (as in Figure 3C) and conversion (as in Figure 3A).
vi. Planned activity for the subsequent reporting period: We will continue using flow cytometry equipment (BD Biosciences: FACS Aria and FACScalibur), antibodies linked to fluorochromes, chemotaxis chambers and cell culture equipment. We will also continue to use the pyrosequencing machines (i.e. Illumina Infinium) available at Stanford for epigenetic research.
We have:
- Completed all collection of samples and clinical outcome measures every 6 months
- Completed our analysis of repeat immune measures (i.e., Treg function, Foxp3 expression, DNA methylation of Foxp3 locus) and repeat clinical outcomes (pulmonary function tests and health questionnaires)on each subject.
- Obtained short-term and long-term individual estimate exposures to ambient air PAHs, PM2.5, black carbon and ozone, and then test whether there is an association of the extent of exposure in each subject to immune outcome measures in the same subject.
- Received notification that our paper was accepted for publication (Hew, et al. 2014).
Journal Articles on this Report : 1 Displayed | Download in RIS Format
| Other project views: | All 9 publications | 4 publications in selected types | All 4 journal articles |
|---|
| Type | Citation | ||
|---|---|---|---|
|
|
Hew KM, Walker AI, Kohli A, Garcia M, Syed A, McDonald-Hyman C, Noth EM, Mann JK, Pratt B, Balmes J, Hammond SK, Eisen EA, Nadeau KC. Childhood exposure to ambient polycyclic aromatic hydrocarbons is linked to epigenetic modifications and impaired systemic immunity in T cells. Clinical & Experimental Allergy 2015;45(1):238-248. |
R834786 (Final) R834596 (2012) R834596 (Final) R834596C003 (Final) R835435 (2014) R835435 (2015) R835435 (2016) R835435 (Final) |
Exit Exit Exit |
Supplemental Keywords:
Human health, air, health effects, biology, health risk assessment, immunology, biochemistry, particulate matter, allergens/asthma, bioavailability, biomarkers, ambient air quality, immune response, human health effects, PM2.5, airborne pollutants, PM10, allergic response, airborne particulate matter, Health, RFA, Scientific Discipline, Air, HUMAN HEALTH, Health Risk Assessment, Immunology, particulate matter, Biology, Allergens/Asthma, Biochemistry, Health Effects, bioavailability, asthma, airborne particulate matter, immune response, PM10, airborne pollutants, allergic response, ambient air quality, human health effects, biomarkersProgress and Final Reports:
Original AbstractThe perspectives, information and conclusions conveyed in research project abstracts, progress reports, final reports, journal abstracts and journal publications convey the viewpoints of the principal investigator and may not represent the views and policies of ORD and EPA. Conclusions drawn by the principal investigators have not been reviewed by the Agency.