Grantee Research Project Results
Final Report: Air Pollution Role in Hypertension and Heart Attacks
EPA Grant Number: R831952Title: Air Pollution Role in Hypertension and Heart Attacks
Investigators: Kleinman, Michael T. , Kloner, Robert
Institution: University of California - Irvine , The Heart Institute of Good Samaritan Hospital
EPA Project Officer: Chung, Serena
Project Period: September 1, 2004 through July 31, 2008 (Extended to August 31, 2009)
Project Amount: $1,534,855
RFA: The Role of Air Pollutants in Cardiovascular Disease (2003) RFA Text | Recipients Lists
Research Category: Particulate Matter , Air Quality and Air Toxics , Air
Objective:
- Determine if exposure to ultra fine (< 0.18 micrometer) particulate matter (UFP) typical of polluted ambient air causes direct physiologic and pathologic damage (not involving the lung) to hearts of healthy individuals or individuals with increased susceptibility due to heart disease or aging.
- Determine whether temporal variations in particle concentrations or chemical compositions induce disturbances of blood pressure, heart rate and heart rate variability (BP, HR and HRV, respectively) in healthy individuals or individuals with increased susceptibility due to heart disease.
- Determine if chronic exposure to polluted ambient air adversely affects the physiology, pathology, and gene expression in the hearts of healthy or susceptible individuals exposed to ambient particulate air pollution.
Summary/Accomplishments (Outputs/Outcomes):
To accomplish the project objectives, we conducted chronic inhalation studies with animal models (in vivo) to examine damage caused by PM to the heart and changes in heart functions induced by PM exposures. To determine if PM that entered the circulation after inhalation could have direct effects on the heart we performed in vitro studies with isolated perfused hearts and intensively evaluated acute changes in heart functions after instilling UFP into a vein leading into hearts from normal rats, aged rats, spontaneously hypertensive rats and rats with induced myocardial infarctions.For the in vivo studies we exposed rats to PM in Riverside, California, a city with hourly average PM concentrations that ranged from about 30 to a peak of 655 µg/m3 during the July through October 2003 period, a time when photochemical activity in the atmosphere was high. The exposures were performed using a particle concentrator, a device that increased the ambient concentrations of PM by about 10-fold, while removing, or greatly reducing, the concentrations of toxic gases such as nitrogen dioxide or ozone. Although the main focus of the research was on UFP ( ≤ 0.18 μm), we also included exposures to fine particles (FP; ≤ 2.5 μm) and coarse particles (CP; 2.5 ≤ dp ≤ 10 μm).
During the in vivo studies we monitored and recorded the electrocardiograms (ECGs), blood pressure and activity levels of rats during their exposures to UFP using surgically implanted devices and used radio telemetry to collect the data. Acute and chronic changes in blood pressure, heart rate, abnormal heart rhythms, and heart rate variability (HRV) were acquired on an hourly and daily basis and related to temporal variations in chemical and physical characteristics of the exposure atmosphere. After the exposures were completed, the hearts and lungs of these animals were examined for adverse pathological changes, blood plasma was examined for the presence of biomarkers that have been associated with heart diseases and gene expression differences in the hearts of normal and susceptible models were determined to evaluate whether the physiological effects were associated with other clinical findings.Conclusions:
Objective 1: Determine if exposure to ultra fine (< 0.18 micrometer) particulate matter (UFP) typical of polluted ambient air causes direct physiologic and pathologic damage (not involving the lung) to hearts of healthy individuals or individuals with increased susceptibility due to heart disease or aging.
Objective 2: Determine whether temporal variations in particle concentrations or chemical compositions induce disturbances of blood pressure, heart rate and heart rate variability (BP, HR and HRV, respectively) in healthy individuals or individuals with increased susceptibility due to heart disease.
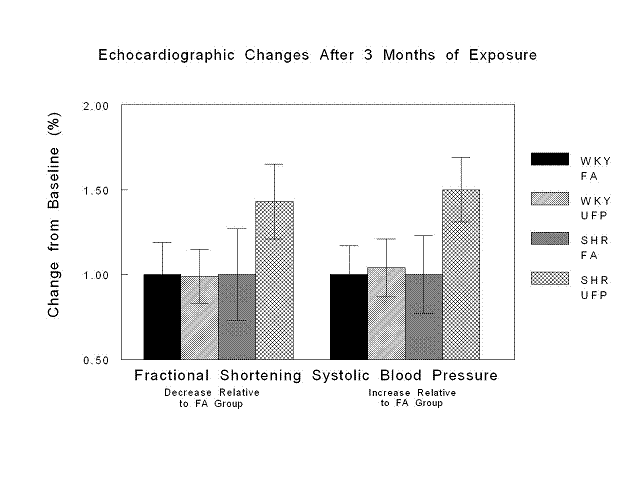
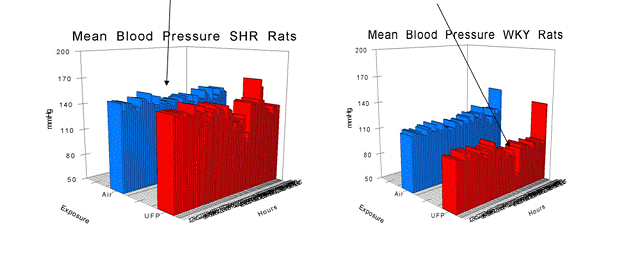
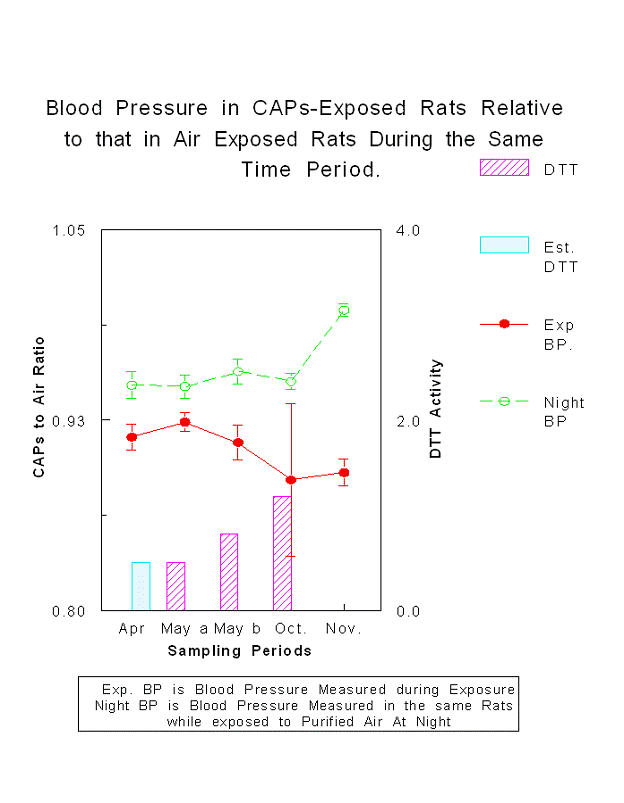
The heart rate (HR), blood pressure (BP) and heart rate variability (HRV) results demonstrated that exposure exacerbated hypertension in SHR rats (measured as mean arterial pressure) but the WKY rats actually demonstrated lower mean arterial BP after 3 months of exposure compared to rats exposed to purified air. At the beginning of exposures the CAPs-exposed SHR rats showed a normal pattern of heart rate compensation for the elevated BP but by the end of the exposure experiment there was evidence that compensation was compromised.


Objective 3. Determine if chronic exposure to polluted ambient air adversely affects the physiology, pathology, and gene expression in the hearts of healthy or susceptible individuals exposed to ambient particulate air pollution.
|
|
|||
|
Component
|
UFP
|
FP
|
CP
|
|
Mass (mg/m3)
|
63 ± 8
|
149 ± 24
|
58 ± 7
|
|
Number (particles/cm3 x 103)
|
65 ± 5
|
67 ± 6
|
*
|
|
EC Mass (μg/m3)
(%)
|
5.5 ± 1.1
8.7
|
6.3 ± 1.1
4.3
|
2.3 ± 0.7
3.9
|
|
OC Mass (μg/m3)
(%)
|
35.8 ± 2.1
56.5
|
38.3 ± 2.6
25.8
|
30.0 ± 1.6
51.4
|
|
|
|||
Journal Articles on this Report : 8 Displayed | Download in RIS Format
| Other project views: | All 18 publications | 8 publications in selected types | All 8 journal articles |
|---|
| Type | Citation | ||
|---|---|---|---|
|
|
Hwang H, Kloner RA, Kleinman MT, Simkhovich BZ. Direct and acute cardiotoxic effects of ultrafine air pollutants in spontaneously hypertensive rats and Wistar-Kyoto rats. Journal of Cardiovascular Pharmacology and Therapeutics 2008;13(3):189-198. |
R831952 (Final) |
Exit |
|
|
Kleinman MT, Araujo JA, Nel A, Sioutas C, Campbell A, Cong PQ, Li H, Bondy SC. Inhaled ultrafine particulate matter affects CNS inflammatory processes and may act via MAP kinase signaling pathways. Toxicology Letters 2008;178(2):127-130. |
R831952 (Final) R832413 (2007) R832413 (2008) R832413 (2009) R832413 (Final) R832413C001 (2007) R832413C001 (2008) R832413C001 (Final) |
Exit Exit Exit |
|
|
Simkhovich BZ, Marjoram P, Kleinman MT, Kloner RA. Direct and acute cardiotoxicity of ultrafine particles in young adult and old rat hearts. Basic Research in Cardiology 2007;102(6):467-475. |
R831952 (Final) |
Exit |
|
|
Simkhovich BZ, Kleinman MT, Kloner RA. Air pollution and cardiovascular injury epidemiology, toxicology, and mechanisms. Journal of the American College of Cardiology 2008;52(9):719-726. |
R831952 (2005) R831952 (Final) |
Exit Exit Exit |
|
|
Simkhovich BZ, Kleinman MT, Kloner RA. Particulate air pollution and coronary heart disease. Current Opinion in Cardiology 2009;24(6):604-609. |
R831952 (Final) |
Exit |
|
|
Simkhovich BZ, Kleinman MT, Willet P, Gookin G, Salazar K, Keebaugh A, Kloner RA. Chronically inhaled ambient particles cause cardiac inflammation in normal, diseased, and elderly rat hearts. Air Quality Atmosphere and Health 2011;4(1):27-36. |
R831952 (Final) |
Exit |
|
|
Simkhovich BZ, Kleinman MT, Mehrian-Shai R, Hsu YH, Meacher D, Gookin G, Kinnon MM, Salazar K, Willet P, Feng G, Lin SM, Kloner RA. Chronic exposure to ambient particulate matter alters cardiac gene expression patterns and markers of oxidative stress in rats. Air Quality Atmosphere and Health 2011;4(1):15-25. |
R831952 (Final) |
Exit |
|
|
Wold LE, Simkhovich BZ, Kleinman MT, Nordlie MA, Dow JS, Sioutas C, Kloner RA. In vivo and in vitro models to test the hypothesis of particle-induced effects on cardiac function and arrhythmias. Cardiovascular Toxicology 2006;6(1):69-78. |
R831952 (2005) R831952 (Final) R827352 (Final) R832413 (2008) R832413 (Final) R832413C001 (2007) R832413C001 (Final) |
Exit |
Supplemental Keywords:
Relevant Websites:
NoneProgress and Final Reports:
Original AbstractThe perspectives, information and conclusions conveyed in research project abstracts, progress reports, final reports, journal abstracts and journal publications convey the viewpoints of the principal investigator and may not represent the views and policies of ORD and EPA. Conclusions drawn by the principal investigators have not been reviewed by the Agency.
