Grantee Research Project Results
2019 Progress Report: The Columbia Center for Childrens Environmental Health
EPA Grant Number: R836154Center: Southern California Children's Environmental Health Center
Center Director: McConnell, Rob Scot
Title: The Columbia Center for Childrens Environmental Health
Investigators: Perera, Frederica P.
Current Investigators: Perera, Frederica P. , Rauh, Virginia , Rundle, Andrew , Peterson, Bradley S , Shepard, Peggy , Hernandez, Diana
Institution: Columbia University in the City of New York
EPA Project Officer: Callan, Richard
Project Period: September 1, 2015 through August 31, 2019 (Extended to August 31, 2020)
Project Period Covered by this Report: September 1, 2018 through August 31,2019
Project Amount: $2,552,707
RFA: Children's Environmental Health and Disease Prevention Research Centers (2014) RFA Text | Recipients Lists
Research Category: Children's Health , Endocrine Disruptors , Human Health
Objective:
Project 1- The Impact of PAH Exposure on Adolescent Neurodevelopment: Disruption of SelfRegulatory Processes
During this project period, we aimed to continue recruitment, scheduling, and assessment activities related to neuropsychological and clinical functioning in the adolescent subjects and their mothers. These objectives are consistent with Specific Aim 1 (to assess the effects of prenatal PAH exposure on neuropsychological performance at 15-17 years of age) and Specific Aim 2 (to assess the effects of prenatal PAH exposure on clinical outcomes at 15-17 years of age in the same adolescents). In addition, we have conducted data cleaning and data entry, in preparation for analysis of the neuropsychological and clinical data in relation to PAH exposure levels. We are now poised to conduct tests of the major hypotheses related to Aims 1 and 2. Aim 3 requires the integration of newly acquired with previously collected data to tests hypotheses related to trajectories over time, and we are now posed to test these hypotheses using neuropsychological and clinical outcome data. In preparation for the integration of data across projects (Aim 4), we have successfully completed N= 295. N=7 participants refused the MRI, N=6 had unsuccessful MRIs, and N=14 could not be imaged because of braces on the teeth.
Project 2- The Impact of PAH Exposure on Childhood Growth Trajectories and Visceral Adipose Tissue Mass in Adolescence: Linkages to Disrupted Self-Regulatory Processes
During this project period, we will complete the recruitment and assessment activities related to diet, physical activity, and anthropometric assessment in the remaining 5 teen subjects and their mothers needed to complete our recruitment goals.
Project 3: An MRI Study of the Effects of Prenatal and Early Childhood PAH Exposure on Brain Maturation and Its Mediating Influences on Adverse Adolescent Outcomes
In Year 4, we focused on the following objectives: (1) Statistical analysis of Magnetic Resonance Imaging (MRI) data for ages 9-12 years in our cohort. We have done this especially for anatomical MRI, Arterial Spin Labeling (ASL) perfusion, DRI, and Magnetic Resonance Spectroscopy (MRS) data; (2) Integration of these MRI data with the demographic, behavioral, and cognitive data acquired at ages 9-12 years, particularly in analyses of the ways in which prenatal PAH exposure levels moderate the association of MRI with cognitive and behavioral measures, and how MRI-based brain measures mediate the association of PAH with cognitive and behavioral measures; (3) Continued processing of anatomical brain imaging data as soon after collected as possible. (4) In addition, we have conducted many of the same analyses in each MRI modality using geospatial modeling-based estimates of prenatal PM2.5 exposure, covarying for prenatal PAH exposure and other potential confounders, to understand how PM2.5 and PAH separately affect brain development.
Progress Summary:
Project 1- These objectives are consistent with Specific Aim 1, where we assess the effects of prenatal PAH exposure on neuropsychological performance at 15-17 years of age, and Specific Aim 2, where we assess the effects of prenatal PAH exposure on clinical outcomes at 15-17 years of age in the same adolescents. In relation to Specific Aim 3, preliminary results have shown significant inverse effects of PAH air concentrations on a measure of inhibitory control at 12-14 years of age, as measured by the NEPSY-II, which assesses neuropsychological development, with no association or interaction with early life stress (see below for composite index of stress). The association with PAH remains significant controlling for environmental tobacco smoke (ETS), sex, gestational age, maternal IQ, maternal education, HOME caretaking, heating season, ethnicity, cotinine, lead, and chlorpyrifos. Now that the MRIs are almost completed, the investigators will be working with Dr. Peterson to determine whether or not there is any mediation by the brain parameters. For Specific Aim 4, we are now addressing the cross-study integrative questions, having resolved questions related to outliers and covariates. Dr. David Pagliaccio, CDI, has continued to work with Drs. Rauh and Margolis to develop hypotheses for analyses and publication. David is interested in pursuing questions regarding anxiety, depression, allostatic load, and stressful experiences, and how environmental exposures may moderate effects of early life adversity on emotional development and brain connectivity. He created an early life stress composite measure, using 5-year data. On this measure, greater early life stress predicts greater CBCL symptomology (internalizing and externalizing) at age 11 and is moderated by PAH exposure, such that the positive association between early life stress and symptoms is stronger among those with more PAH exposure. This holds up when controlling for ETS, sex, gestational age, maternal IQ, maternal education, HOME caretaking, heating season, ethnicity, cotinine, lead, and chlorpyrifos. The resulting paper received positive reviews and is now in revision in a high impact journal.
Project 2- The Impact of PAH Exposure on Childhood Growth Trajectories and Visceral Adipose Tissue Mass in Adolescence: Linkages to Disrupted Self-Regulatory Processes
In our fourth year, we have continued to recruit and enroll study subjects at ages 15 to 18 and have completed 295 evaluations for Project 2 and so are very close to reaching our goal of 300 participants. We have been collecting data on physical activity, hedonic eating, food insecurity, height, weight, waist circumference, % body fat, and blood pressure from the teens and their mothers. We have also been collecting data on weight cycling, weight loss practices and weight loss surgery from the mothers, and resting heart rate and heart rate recovery after a step test from the teens. Further, the teens have been undergoing MRI scans of the abdomen to measure visceral abdominal fat. We have completed and published analyses of prenatal exposure to PAH and BMI Z-score trajectories from age 5 to age 14. We found that at age 5, BMI Z-scores were significantly greater for children in the third tertile of exposure relative to the first tertile (0.35 Z-score units, 95% CI 0.09, 0.61, p = 0.007) and were non-significantly higher for the second tertile of exposure compared to the first tertile (0.25 Z-score units, 95% CI -0.02, 0.52, P = 0.075). The trajectories of BMI Z-scores by tertiles of exposure converged as the children aged, such that by age 11 years the estimated mean BMI Z-scores associated with each tertile of exposure were not different. As such prenatal exposures to airborne PAH were associated with higher childhood BMI Z-scores at a young age, but growth trajectories converged by age 11 years. Accordingly, highly exposed children spend a greater proportion of their childhood with higher BMI Z-scores. We have completed preliminary data analyses for the Visceral Adipose Tissue (VAT), Subcutaneous Adipose Tissue (SAT), Intra- & inter- Muscular Adipose Tissue (IMAT) and Abdominal Muscle Tissue (Muscle) measures derived from the first 140 abdominal MRI scans for study subjects age 15-20. Compared to African American participants, the Dominican participants had significantly higher VAT, SAT and IMAT, but similar Muscle. Maternal pregnancy obesity and excessive gestational weight gain were both associated with higher VAT, SAT, IMAT, and Muscle. Prenatal exposures to PAH were not associated with differences in VAT, SAT, IMAT, and Muscle at age 15-17. Higher scores for the DESR scale, indicating poorer emotional self-regulation, were associated with significantly higher amounts of Muscle and non-significantly higher amounts of VAT, SAT, and IMAT (Aim 4). These preliminary analyses will be re-done once we have completed data collection and have reached our target goal of 300 MRI scans. We have also conducted preliminary analyses of maternal and teen reported food insecurity and BMI and the MRI derived body composition measures for the first 217 participants. Among boys, but not among girls, the self-report of food insecurity is associated with lower VAT and IMAT with borderline statistical significance. There were no associations between maternal reported food insecurity and teen BMI Z-scores or body composition measures. These analyses were presented at the 2019 meeting of the American Association of Public Health. These preliminary analyses will be re-done once we have completed data collection and have reached our target goal of 300 MRI scans. We have completed analyses of phthalate metabolites in maternal urine samples collected during pregnancy and child BMI Z-score trajectories from age 5 to 14 years. Our previously published analyses found that higher non-DEHP metabolites were associated with lower BMI Z-score and fat mass index among girls at ages 5 and 7 and were unassociated with BMI Z-scores and fat mass index among boys. Our new trajectory based analyses are consistent with these past findings and show that higher nonDEHP metabolites are associated with lower BMI Z-scores in girls through age 14 and are unassociated with BMI Z-scores among boys through age 14. As in our past analyses at age 5 and 7 DEHP metabolites are not associated with BMI Z-scores in boys and girls. A report on this work is being written for journal publication. Dr. Peterson will soon begin analyzing MRI data collected age 9-11 on brain structure and function in relation to anthropometric data collected at the same time point (Aim 4). In support of these analyses, Drs. Rundle and Goldsmith identified possible relevant confounding variables for the analyses of the anthropometric data, assessed missing covariate data and implemented a multiple imputation strategy using Multiple Imputation by Chained Equations (MICE) to impute missing covariate values. Five sets of data with anthropometric data and covariate data, with imputed values for missing covariate data, were created and sent to Dr. Peterson for analyses with the MRI scan data. Dr. Eliza Kinsey, a post-doctoral scholar in the Department of Epidemiology, wrote a K99R00 Career Development Application to study food insecurity and child obesity and neurodevelopment outcomes in the cohort. Her application received a score of 20.
Project 3
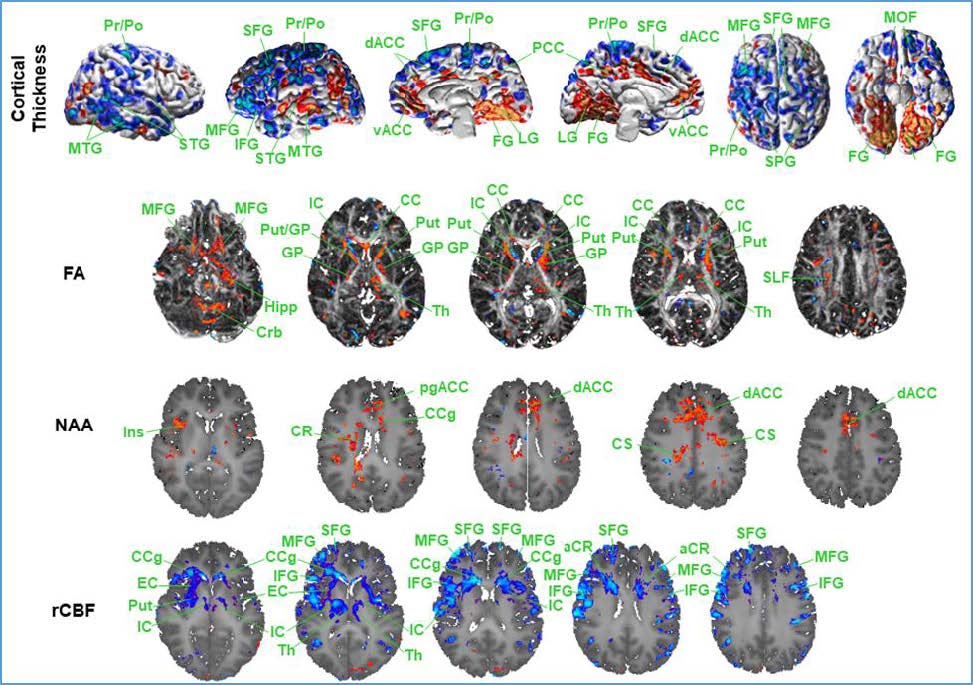
Fig.1 Exposure-Related Effects of Prenatal PAH Exposure on Brain Measures at Ages 9-12 Years Top Row: Anatomical MRI for measures of cortical thickness. Second Row: DTI for measures of fractional anisotropy (FA). Third Row: MR Spectroscopy for measures of N-acetylaspartate (NAA). Bottom Row: Arterial Spin Labeling measures of regional cerebral blood flow (rCBF). The red areas indicate a positive correlation and the blue areas indicate an inverse correlation.
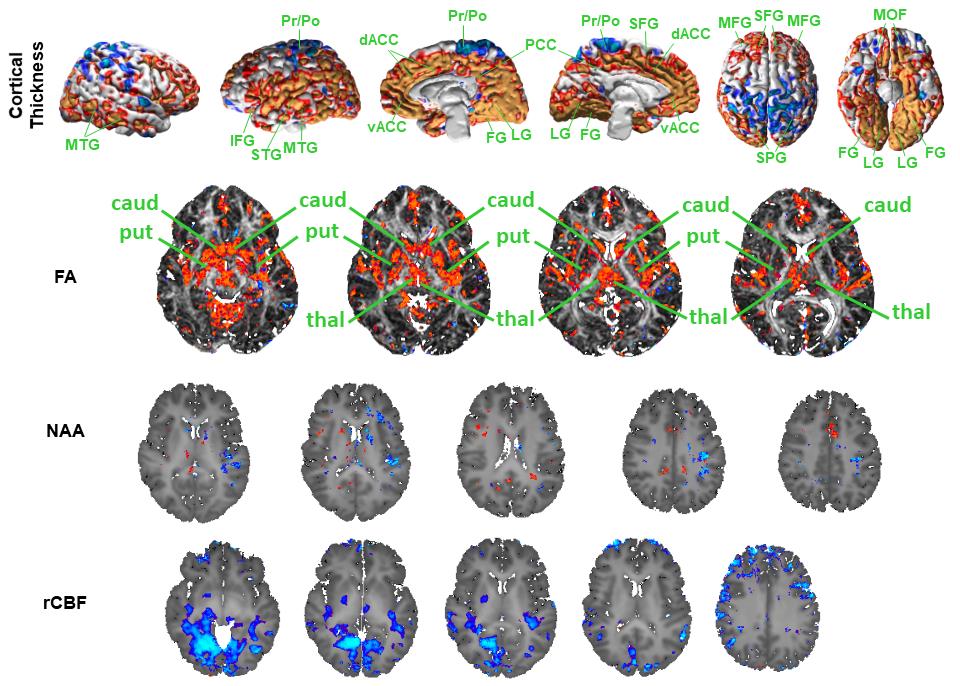
Figure 2: Exposure-Related Effects of Prenatal PM2.5Exposure on Brain Measures at Ages 9-12 Years Top Row: Anatomical MRI for measures of cortical thickness. Second Row: DTI for measures of fractional anisotropy (FA). Third Row: MR Spectroscopy for measures of N-acetylaspartate (NAA). Bottom Row: Arterial Spin Labeling measures of regional cerebral blood flow (rCBF). The red areas indicate a positive correlation and the blue areas indicate an inverse correlation.
We have learned that PAH and PM2.5 exert very different effects on brain development across all MRI modalities.Anatomical MRI: Prenatal PAH exposure (Fig.1) is associated with cortical thinning (blue) in the lateral and dorsal medial surfaces of the brain and thickening in the inferior medial and ventral surfaces of the brain. Prenatal PM2.5 exposure (Fig.2), in contrast, is associated with cortical thickening in most surfaces of the brain, the exceptions being a small amount of exposure-related thinning in the dorsal surfaces of the brain, especially in the dorsal right hemisphere. DTI: Prenatal PAH exposure was associated with higher fractional anisotropy (FA) values in both deep white matter tracts (internal capsule, external capsule) that interconnect the basal ganglia with frontal lobes of the brain, as well as increased FA in some portions of the basal ganglia nuclei and thalamus (Fig.1). Prenatal PM2.5 exposure, on the other hand, was most prominently associated with higher FA values in gray matter nuclei of the basal ganglia and thalamus (Fig.2). MRS: Prenatal PAH exposure was associated with higher NAA concentrations in primarily gray matter portions of the dorsal anterior cingulate gyrus, a locus of executive functioning in the brain (Fig.1). Prenatal PM2.5 exposure, in contrast, was not strongly associated with NAA concentrations. Perfusion: Prenatal PAH exposure was associated with reduced regional cerebral blood flow (rCBF) primarily in frontal regions of the brain in both gray and white matter (Fig.1). Prenatal PM2.5 exposure was associated with reduced rCBF in ventral surfaces of the brain and, to a lesser extent, in more dorsal portions of frontal gray matter (Fig.2) We have also found that sex of the participant powerfully moderates some of these associations of PAH and PM2.5 exposure with brain measures; as a rather crude generalization, the effects of PAH seem to be stronger in females, whereas the effects of PM2.5 exposure are stronger in males (results not shown). In addition, prenatal PAH exposure powerfully moderates the associations of brain measures with neurocognitive and behavioral outcomes (also not shown). We are in the process of conducting tests of moderated mediation, hypothesizing that PAH exposure produces a phenocopy of behavioral disturbances (such as ADHD) through different brain pathways than those that produce ADHD that is not a consequence of prenatal PAH exposure. For collection and processing data for Specific Aim 3, the quality of anatomical brain images acquired under the auspices of the P50 has been superb. Processing of the anatomical images is keeping pace with the rate of scan acquisition. We will be ready to statistically analyze these images quickly, as soon as data collection stops.
Future Activities:
Project 1
During the No Cost Extension period we will complete the follow-up of the cohort. Although we have reached our target enrollment goal for the neuropsychological and clinical assessments, we aim to complete 5 more MRIs. The recruitment and data collection procedures will continue to follow protocols that we originally stipulated in our grant application. During the upcoming no cost extension period, an additional number of participants have recently turned, or will soon turn 15 years old, and will age into the eligible assessment window.
Project 2
In the coming reporting period we will complete enrollment and data collection from the cohort participants at age 15-17 years. The data analyses in support of Aims 1-4 will be conducted in collaboration with Drs. Perera, Rauh, Peterson and Goldsmith.
Project 3
We are focusing on writing the manuscripts reporting the above findings for the age 9-12 MRI findings. We will soon begin statistical analyses as described in the grant application. We are completing the moderated mediation analysis for the PAH findings, and have begun mediation analyses for the PM2.5 exposure estimates. We anticipate these findings to lead to publication in highimpact journals. Our publication in the J Neuroscience (above) has identified the brain systems that mature rapidly in the years from 9-12 and the mediate improved self-regulation at those ages. Our preliminary findings above suggest that PAH in particular, but also PM2.5, disrupts development of those neural systems.
Journal Articles: 10 Displayed | Download in RIS Format
| Other center views: | All 13 publications | 10 publications in selected types | All 10 journal articles |
|---|
| Type | Citation | ||
|---|---|---|---|
|
|
Conrad L, Rauh V, Hopener L, Acosta L, Perera F, Rundle A, Arteaga-Solis E, Miller R, Perzanowski M. Report of prenatal maternal demoralization and material hardship and infant rhinorrhea and watery eyes. Annals of Allergy Asthma & Immunology 2020;125(4):399. |
R836154 (2019) R832144 (Final) |
Exit |
|
|
Durham T, Guo J, Cowell W, Riley K, Wang S, Tang D, Perera F, Herbstman J. Prenatal PM2.5 Exposure in Relation to Maternal and Newborn Telomere Length at Delivery. Toxics 23;10(1):13. |
R836154 (Final) R827027 (2002) R832141 (Final) R834509 (Final) |
Exit Exit |
|
|
Flores N, Lovinsky-Desir S, Divjan A, Hoepner L, Zou J, Miller R, Herbstman J, Perera F, Perzanowski M, Checn Q. Trajectory analysis of rhinitis in a birth cohort from lower-income New York City neighborhoods. JOURNAL OF ALLERGY AND CLINICAL IMMUNOLOGY 2024;154(1) |
R836154 (Final) |
Exit |
|
|
Hoepner LA, Whyatt RM, Widen EM, Hassoun A, Oberfield SE, Mueller NT, Diaz D, Calafat AM, Perera FP, Rundle AG. Bisphenol A and adiposity in an inner-city birth cohort. Environmental Health Perspectives 2016;124(10):1644-1650. |
R836154 (2017) R834509 (Final) |
|
|
|
Hopson MB, Margolis A, Rauh V, Herbstman JB. Impact of the home environment on the relationship between prenatal exposure to environmental tobacco smoke and child behavior. International Journal of Child Health and Human Development 2016;9(4):453-464. |
R836154 (2017) |
|
|
|
Maresca MM, Hoepner LA, Hassoun A, Oberfield SE, Mooney SJ, Calafat AM, Ramirez J, Freyer G, Perera FP, Whyatt RM, Rundle AG. Prenatal exposure to phthalates and childhood body size in an urban cohort. Environmental Health Perspectives 2015 June 12 [Epub ahead of print], doi:10.1289/ehp.1408750. |
R836154 (2017) R834509 (2013) R834509C001 (Final) |
|
|
|
Margolis AE, Herbstman JB, Davis KS, Thomas VK, Tang D, Wang Y, Wang S, Perera FP, Peterson BS, Rauh VA. Longitudinal effects of prenatal exposure to air pollutants on self-regulatory capacities and social competence. Journal of Child Psychology and Psychiatry 2016;57(7):851-860. |
R836154 (2017) R834509 (Final) |
Exit Exit |
|
|
Perera FP, Wheelock K, Wang Y, Tang D, Margolis AE, Badia G, Cowell W, Miller RL, Rauh V, Wang S, Herbstman JB. Combined effects of prenatal exposure to polycyclic aromatic hydrocarbons and material hardship on child ADHD behavior problems. Environmental Research 2018;160:506-513. |
R836154 (2017) R836154 (2018) |
Exit Exit Exit |
|
|
Perera F, Nolte ELR, Wang Y, Margolis AE, Calafat AM, Wang S, Garcia W, Hoepner LA, Peterson BS, Rauh V, Herbstman J. Bisphenol A exposure and symptoms of anxiety and depression among inner city children at 10-12 years of age. Environmental Research 2016;151:195-202. |
R836154 (2017) |
Exit Exit Exit |
|
|
Widen EM, Whyatt RM, Hoepner LA, Mueller NT, Ramirez‐Carvey J, Oberfield SE, Hassoun A, Perera FP, Gallagher D, Rundle AG. Gestational weight gain and obesity, adiposity and body size in African-American and Dominican children in the Bronx and Northern Manhattan. Maternal & Child Nutrition 2016;12(4):918-928. |
R836154 (2017) R834509C001 (Final) |
Exit |
Progress and Final Reports:
Original Abstract Subprojects under this Center: (EPA does not fund or establish subprojects; EPA awards and manages the overall grant for this center).
R836154C001 The Impact of PAH Exposure on Adolescent Neurodevelopment: Disruption of Self-Regulatory Processes
R836154C002 The Impact of PAH Exposure on Childhood Growth Trajectories and Visceral Adipose Tissue
R836154C003 An MRI Study of the Effects of Prenatal and Early Childhood PAH Exposure on Brain Maturation and Its Mediating Influences on Adverse Adolescent Outcomes
The perspectives, information and conclusions conveyed in research project abstracts, progress reports, final reports, journal abstracts and journal publications convey the viewpoints of the principal investigator and may not represent the views and policies of ORD and EPA. Conclusions drawn by the principal investigators have not been reviewed by the Agency.