Grantee Research Project Results
Final Report: Responses to Fresh Aerosol in Susceptible Subjects
EPA Grant Number: R832144Title: Responses to Fresh Aerosol in Susceptible Subjects
Investigators: Kipen, Howard , Lioy, Paul J. , Philipp, Claire , Shindler, Daniel , Laskin, Deborah , Zhang, Junfeng , Ohman-Strickland, Pamela , Laumbach, Robert , Fan, Tina
Institution: Robert Wood Johnson Medical School
EPA Project Officer: Chung, Serena
Project Period: October 1, 2004 through September 30, 2008
Project Amount: $1,521,398
RFA: The Role of Air Pollutants in Cardiovascular Disease (2003) RFA Text | Recipients Lists
Research Category: Particulate Matter , Air Quality and Air Toxics , Air
Objective:
Summary/Accomplishments (Outputs/Outcomes):
1) Phenotypic Changes in Platelet Activation Using Surface Markers
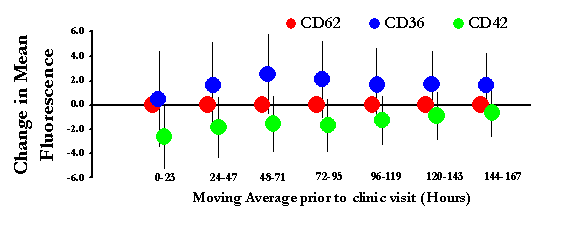 Figure
Figure
2. Plasma Nitrite Assessment
Since design of our study, blood nitrite (NO2) has been reported as an alternative to brachial artery ultrasound scanning (BAUS) and Endo-PAT measurement as a marker of endothelial function (Allen et al, 2005). As a biochemical marker, it is reasonable to examine it in concert with the other, more physiological markers, as it is felt to underlie the physiological vasodilation. We initiated these studies as a consequence of the difficulty we had with the BAUS technique. We have collected blood samples from 49 subjects for measurement of nitrite levels at baseline (pre-exposure) and following a 2-hour exposure to diesel exhaust particles (DE), secondary organic aerosols (SOA), and clean air (CA). Due to restrictions of available staff time required to analyze samples, samples collected on the SOA day are not analyzed. Post minus pre exposure difference for nitrite levels (diff-CA-Nitrite, diff-DE-Nitrite) was calculated for DE and CA days (see 2008-2009 report). These results show, as hypothesized, a greater decrease in nitrite following DE exposure than following exposure to CA. However, there were no statistically significant differences between responses on DE and CA days.
|
|
Outcome variable
|
Pre CA
(N=49)
|
Post* CA
(N=48)
|
6 hrs post CA (N=47)
|
Pre DE
(N=46)
|
Post*DE
(N=45)
|
6 hrs post
DE (N=45)
|
|
WBC count (Thous/mcL)
|
6.7 (1.4)
|
6.6 (1.5)
|
6.7 (1.5)
|
6.7 (1.5)
|
6.7 (1.7)
|
6.6 (1.6)
|
|
RBC count (Thous/mcL)
|
4.7 (0.4)
|
4.9 (0.5)
|
4.7 (0.4)
|
4.7 (0.4)
|
4.9 (0.4)
|
4.7 (0.4)
|
|
Race
|
HET
|
HOM
|
WT
|
UNDETERMINED
|
Total
|
|
White
|
274 (94.8%)
|
48 (96%)
|
283 (86.8%)
|
21 (95.4%)
|
626 (91.1%)
|
|
Black
|
0 (0%)
|
1 (2%)
|
3 (0.9%)
|
0 (0%)
|
4 (0.587%)
|
|
Asian
|
13 (4.5%)
|
1 (2%)
|
35 (10.7%)
|
1 (4.5%)
|
50 (7.2%)
|
|
Other
|
2 (0.6%)
|
0 (0%)
|
5 (1.5%)
|
0 (0%)
|
7 (1.0%)
|
|
Total
|
289 (42%)
|
50 (7.2%)
|
326 (47.4%)
|
22 (3.2%)
|
687 (100%)
|
|
Race
|
HET
|
HOM
|
WT
|
Total
|
||||||||||||||||||||||||||||||||||||||||
|
White
|
18 (75%)
|
14 (100%)
|
14 (56%)
|
46 (73%)
|
||||||||||||||||||||||||||||||||||||||||
|
Black
|
0 (0%)
|
0 (0%)
|
1 (4%)
|
1 (1.5%)
|
||||||||||||||||||||||||||||||||||||||||
|
Asian
|
5 (20.8%)
|
0 (0%)
|
10 (40%)
|
15 (23.8%)
|
||||||||||||||||||||||||||||||||||||||||
| We have presented selected results above. None of these data can yet be considered fully vetted and complete, in particular the cellular platelet activation and blood nitrite data. However, in general, results from the DE and SOA exposures led to less dramatic and less significant changes than we had hypothesized. We did not clearly demonstrate inflammation, a major hypothesis to explain air pollution effects on CVD, from our system using conventional assays on either peripheral blood or the lung. It remains possible that our exposures were less potent than those in some other systems for particle exposure.
We have been hampered in obtaining BAUS measurement on the intended number of subjects, but in conjunction with the nitrite/nitrate data no strong signal for endothelial dysfunction from the DE condition has emerged. EndoPAT did not prove a reliable alternative to BAUS for our acute studies. Significant platelet activation changes do not appear likely, with our analytical cytometry data supported by the absence of significant changes in the soluble marker data. Once our phenotypic results are confirmed, we will further explore individual genetic susceptibility, although power will be limited as we are restricted to 14 homozygous variant subjects. Ambient air effects on platelet activation are promising but will require confirmation. UPP is our only clearly significant finding and we are exploring its implications, in particular its key role as a regulator of the oxidative stress response. It was statistically significant only when both SOA and DE conditions were combined, although both exposures were associated with decreases in activation compared to clean air in these within-subject analyses..
We have used the experience and results of this study to date as preliminary data for a new NIEHS R01 (ES015864) awarded to Dr. Zhang with Dr. Kipen as Co-I: Response to Drastic Changes in Air Pollution: Reversibility and Susceptibility. We have completed data collection for this project and are now in the analysis phase. A direct extension of the current study (Gene x Environment Interactions after Diesel Exhaust Inhalation in Humans), emphasizing more detailed genotyping of the subjects, as well as additional outcome collection on 35 more subjects, was submitted as an NIH Challenge Grant, but this has not received funding through the main NIH channel.
In collaboration with epidemiologist David Rich we are analyzing additional selected baseline parameters as discussed above (platelet activation, blood counts, EndoPAT) against outdoor ambient air pollution, searching for an association between preceding PM levels and the specified outcomes. This is one way to address the possibility that our diesel exposure is somehow different than those in studies that have reported more robust physiological effects of diesel exhaust.
References:Allen JD, Cobb FR, Gow AJ. Regional and whole-body markers of nitric oxide production following hyperemic stimuli. Free Radic Biol Med. 2005 May 1;38(9):1164-9.
Lucking AJ, Lundback M, Mills NL, Faratian D, Barath SL, Pourazar J, Cassee FR, Donaldson K, Boon NA, Badimon JJ, Sandstrom T, Blomberg A, Newby DE . Diesel exhaust inhalation increases thrombus formation in man.. Eur Heart J. 2008 Dec;29(24):3043-51
Journal Articles on this Report : 9 Displayed | Download in RIS Format
Supplemental Keywords:Diesel exhaust, secondary organic aerosol, endothelial function, platelet activation, cardiovascular disease, vascular nitrite, ubiquitin proteasome pathway (UPP), RFA, Health, Scientific Discipline, Air, HUMAN HEALTH, Susceptibility/Sensitive Population/Genetic Susceptibility, Health Risk Assessment, Risk Assessments, particulate matter, Biology, genetic susceptability, mobile sources, Exposure, Biochemistry, air toxics, air quality, diesel exhaust, inhaled, sensitive populations, environmental hazard exposures, inhaled pollutants, fine particles, human exposure, lung inflammation, oxidant gas, engine exhaust, acute lung injury, DEP, cardiopulmonary responses, particulate exposure, Nitric Oxide Synase, acute exposure, Acute health effects, cardiotoxicity, copollutant exposures, airway epithelial cells, diesel exhaust particulate, chronic health effects, susceptible subpopulations, toxics, concentrated particulate matter, heart rate, air contaminant exposure, atmospheric particulate matter, air pollution, cardiopulmonary, cardiovascular disease, highrisk groups, human health risk, human susceptibility, airborne urban contaminants, ambient particle pollution, automotive exhaust, cardiopulmonary response, diesel exhaust particlesProgress and Final Reports:Original AbstractThe perspectives, information and conclusions conveyed in research project abstracts, progress reports, final reports, journal abstracts and journal publications convey the viewpoints of the principal investigator and may not represent the views and policies of ORD and EPA. Conclusions drawn by the principal investigators have not been reviewed by the Agency. Project Research ResultsSite NavigationRelated InformationContact Us to ask a question, provide feedback, or report a problem.
Last updated April 28, 2023
|
